For Patients
Endometrial cancer
Symptoms
Ninety percent of the patients with endometrial cancer experience atypical genital bleeding. It should be noted that bleeding may be limited to brown vaginal discharge. It is important to visit a gynecologist if genital bleeding persists for a long time or if bleeding occurs even after menopause.
Diagnosis
Endometrial cancer originates in the body of the uterus. It includes endometrial cancer derived from the endometrium and uterine sarcoma in which other parts of the uterus have become malignant. The latter is relatively rare and its differentiation from uterine myoma is challenging.
The diagnosis of endometrial cancer requires to determine "Is there a cancer? If there is, what type of cancer is it? (diagnosis of the presence of endometrial cancer)" and "If there is, how far has it spread? (diagnosis of cancer spread)."
Cytodiagnosis or tissue diagnosis, which involves direct collection of cells and tissues from the endometrium, are commonly used for checking whether there is endometrial cancer. Generally speaking, uterine cancer screening refers to the screening of cervical cancer and not endometrial cancer. It should be noted that the screening for endometrial cancer is usually not included in this screening.
In endometrial cytodiagnosis, cells are collected by inserting a thin apparatus from the opening of uterus. Tissue diagnosis is used when abnormalities are suspected in the cytodiagnosis. It should be noted that endometrial cytodiagnosis is not as accurate as cervical cytodiagnosis.
Tissues are collected in the same way by inserting an apparatus also in tissue diagnosis. The diagnosis can sometimes be impossible in aged women or those who have never given birth, in whom the opening of uterus is narrowed or closed. Enough cells and tissues may not be obtained because of pains. In such cases, diagnoses are sometimes made after the treatments to widen the opening of uterus or applying anesthesia in advance.
Tissues are sometimes collected while observing the inside of the uterus with a scope (hysteroscope). These are the examinations to see if there is endometrial cancer.
An alternative approach is to check the thickness of the endometrium by transvaginal ultrasonography. This is because the endometrium thickens when endometrial cancer develops. Although this approach is useful as a method of screening because it causes less pain, it has some disadvantages including the difficulty in the determination before menopause and overlooking early-stage cancers.
Examinations to check the spread of endometrial cancer include imaging tests such as MRI, CT, and PET-CT. MRI assesses how much the cancer has invaded into the wall of the uterus (muscle invasion) and whether the cancer has spread to the ovary and oviduct adjacent to the uterus. CT and PET-CT assess the presence of metastatic cancer in organs and lymph nodes throughout the body. The results of these assessments serve as important information for deciding the approach of treatments.
Approximately 2-5% of endometrial cancers are of hereditary nature (Lynch syndrome). In this case, cancers may develop at relatively young ages, and cancers such as uterine body, colon, ovarian, and stomach cancers may cluster within a family.
Treatments
Surgery is the main treatment for endometrial cancer. The surgery is mostly the removal of the uterus and the ovaries/oviducts on both sides. Final spread of the cancer (stage of progression) is assessed by removing the lymph nodes (lymph node dissection) to which the cancer metastasizes; however, this procedure is sometimes omitted depending on the type and spread of the cancer. For some early-stage endometrial cancers, laparoscopic surgery using a camera and robot-assisted surgery have also become available as medical treatments covered by health insurance, in addition to conventional laparotomy cutting into the abdomen.
The uterus, ovaries, and lymph nodes removed are examined under a microscope to determine the stage of endometrial cancer progression. Table 1 shows the postoperative staging of endometrial cancer. Chemotherapy with anticancer drugs or radiation therapy is given when the risk of recurrence is considered high based on postoperative assessments. Chemotherapy is often used in Japan. Figure 1 shows 5-year survival rates by the stages of endometrial cancer.
Chemotherapy, radiation therapy, and hormone therapy are usually given in case of cancer recurrence. However, immune checkpoint inhibitors can also be used for some endometrial cancers associated with genetic mutations.
Hormone therapy where the uterus is preserved is also an option for early-stage endometrial cancer in women who wish to become pregnant and in those with uterine body atypical growth, which is regarded as the precancerous lesion of endometrial cancer. However, it is necessary to consult with your doctor because indications and side effects should be considered.
Table 1. Postoperative stage classification of endometrial cancers (Acta Obstetrica et Gynaecologica Japonica (2011), FIGO2008)
| Stage I: Cancers localized to the uterine body | ||||
|---|---|---|---|---|
| Stage IA | Cancers smaller than 1/2 of the myometrium | |||
| Stage IB | Cancers larger than 1/2 of the myometrium | |||
| Stage II: Cancers have invaded the cervical stroma but not extended beyond the uterus* * Those with only cervical gland invasion are stage I rather than stage II. |
||||
| Stage III: Cancers have spread outside the uterus but not extended beyond the small pelvic cavity, or those that have spread to regional lymph nodes | ||||
| Stage IIIA | Cancers that affect the uterine serosa and/or the appendages of the uterus | |||
| Stage IIIB | Cancers that spread to the vagina and/or the parametrium tissues | |||
| Stage IIIC | Cancers with metastases to the pelvic lymph nodes and/or the para-aortic lymph nodes | |||
| Stage IIIC1 | Cancers positive for pelvic lymph node metastasis | |||
| Stage IIIC2 | Cancers positive for para-aortic lymph node metastasis with or without pelvic lymph node metastasis | |||
| Stage IV: Cancers that have extended beyond the small pelvic cavity or apparently affected the bladder and/or intestinal mucosa, and/or have distant metastases | ||||
| Stage IVA | Cancers with invasion to the bladder and/or intestinal mucosa | |||
| Stage IVB | Cancers with distant metastases, including intraperitoneal and/or inguinal lymph node metastases | |||
Figure 1. Five-year survival rate by the stages of endometrial cancer
in the patients diagnosed in 2012.
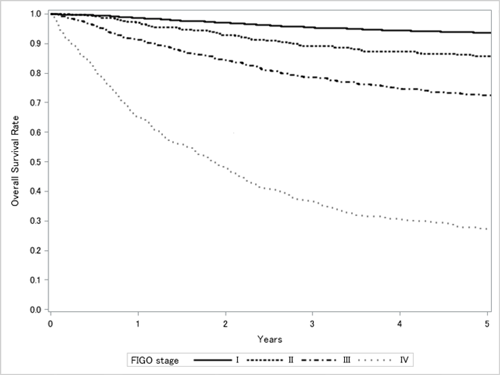
From the report of the Gynecologic Oncology Committee of the Japan Society of Obstetrics and Gynecology, the 60th Annual Treatment Report
(Acta Obstetrica et Gynaecologica Japonica (2019) 71, 758)